Five Questions to Consider if You Think Your Child Might Have Measles
Be sure to call ahead when seeking medical attention if you think your child has measles.
With the rise in measles cases, there will come a time when you think your child might have measles.
Why?
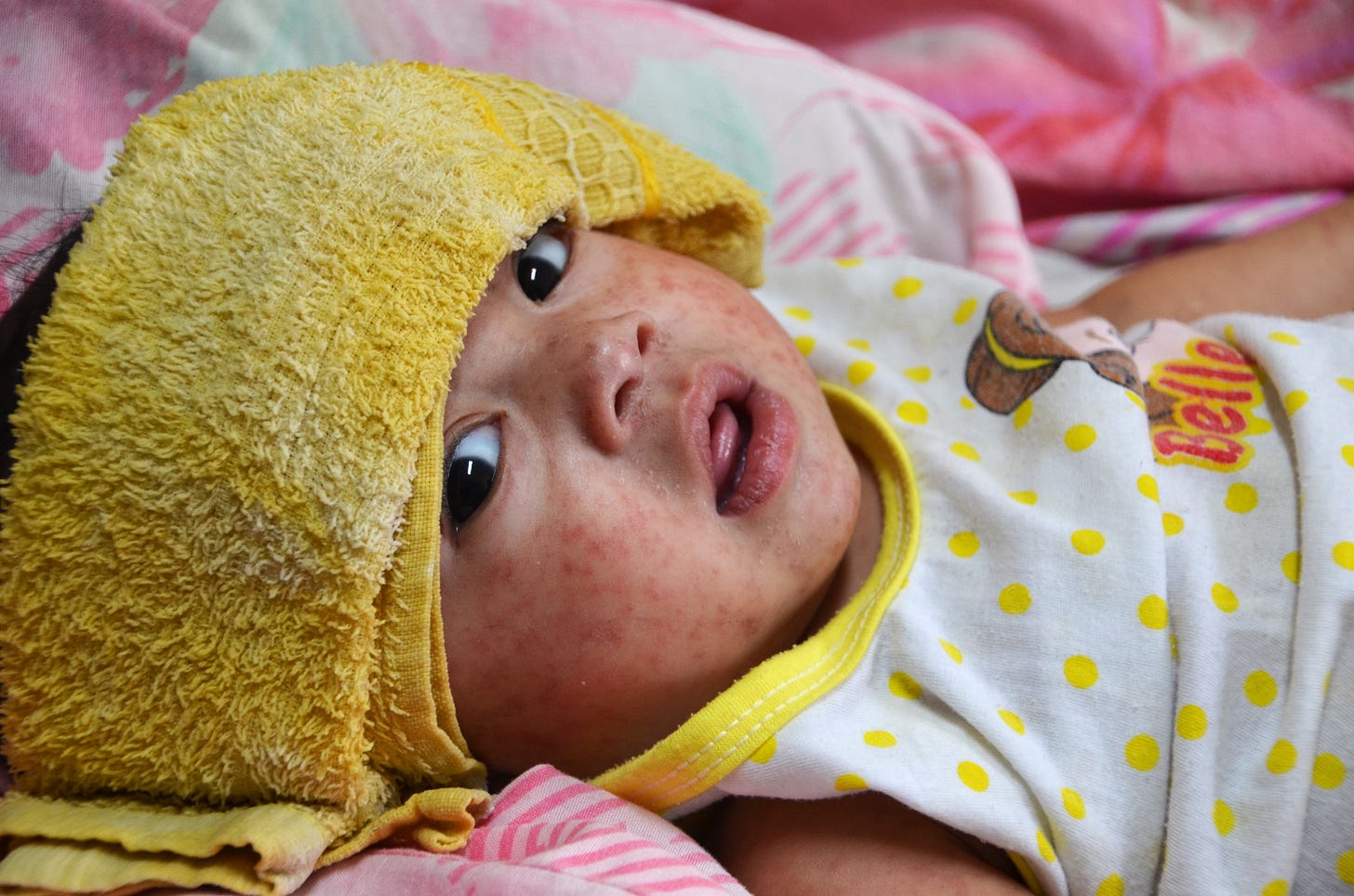
Because a fever and rash are very common symptoms with many childhood diseases!
Fortunately, at least for now, most of the time, it won’t be measles.
From Fifth disease to Roseola, many viral diseases include a fever and rash.
Five Questions to Consider if You Think Your Child Might Have Measles
These five questions will hopefully help you get some idea of how concerned you should be, although you should always call your medical provider if there is any question that your child has been exposed or might have measles:
Has your child received two doses of the MMR vaccine? While that isn’t a guarantee that your child doesn’t have measles, two age-appropriate doses of the MMR vaccine are at least 97% effective at preventing measles infections. Just keep in mind that both doses should have been given after your child turned 12 months old and for best protection, you would hope that it has been at least two weeks between their last dose and your child’s exposure to someone with measles. A dose of MMR given within three days of exposure (post-exposure prophylaxis) might still help, but is less likely to prevent measles. And even if vaccinated, your answer to the next few questions will be important!
Has your child recently traveled out of the country or to an area with an active measles outbreak? Since the incubation period for measles is 7 to 21 days, recent travel to a high risk area, followed by the development of measles symptoms would be very, very suspicious for an acute measles infection.
Has your child recently been exposed to a known case of measles? Again, that would be very suspicious for an acute measles infection, even if they were fully vaccinated.
Has your child recently visited a place or attended an event that could have put them at risk to be exposed to measles, especially situations where you would expect many international visitors or large numbers of people who are unvaccinated? This would put them at increased risk.
What are your child’s symptoms? Remember that measles symptoms can include a high fever, dry cough, runny nose, sore throat, photophobia, irritability and a characteristic rash that begins after 3 to 5 days of fever. And unlike many other viral diseases, once the rash appears, the fever continues for several more days. In fact, the fever often gets worse as the fever appears! So, do your child’s symptoms match the symptoms of measles?
What if your child developed a fever and/or rash about 7 to 12 days after getting an MMR vaccine, without any likely exposure to someone with measles? With a recent MMR vaccine and no likely exposure to measles, especially if your child’s fever is easy to control, it is much more likely that your child is having a simple immune reaction to the MMR vaccine and doesn’t have measles. Contact your pediatrician provider if you have any concerns.
Most importantly, if you truly believe that your child might have measles, call ahead before seeking medical attention.
Why?
Measles is very contagious, and you don’t want to expose anyone else as you seek help for your child - or yourself.
Ideally, while wearing a mask, you will be immediately sent to an airborne infection isolation room (if available) or private room (with the door closed) and not sent through the waiting room.
And remember, as long as you answered yes to question one, you likely won’t have to worry that your child has measles!
References
Minimize Measles Transmission in Health Care Settings. https://www.health.state.mn.us/diseases/measles/hcp/minimize.html

